Reclaiming Movement: My Journey Through Recovery After Glioma Surgery
The Healing Start
Picture this: a bustling neurosurgical center, and there I was, one of 115 patients embarking on a journey that would change everything. From January 2018 to December 2019, I wasn’t just another statistic; I was part of a carefully orchestrated single-center randomized control trial (RCT). The doctors were looking for something—a glimpse into how we could reclaim our lives after craniotomy for glioma resection. I fit the criteria—over 18 years old, no prior surgeries, and yes, I had signed that daunting informed consent form that felt like sealing my fate.
I remember feeling both hopeful and terrified as I learned about the exclusion criteria. No other malignant tumors? Check. Preexisting neurological deficits? Thankfully not. It felt like a mini-application process for life itself, but in many ways, it made me feel seen—not just as a patient but as an individual navigating this intricate dance between fear and hope.
The Right Data
The data collected during this trial wasn’t just numbers or graphs plotted on sterile sheets; they were stories waiting to be told. Diagnostic reports painted pictures of my insides—MRI scans revealing secrets hidden beneath my skull. Each progress note was like a diary entry chronicling my recovery journey: moments of strength followed by waves of exhaustion.
I think back to the primary sources—the hospital discharge records and nursing assessments—they weren’t merely protocols; they were lifelines. They captured not just medical facts but the essence of what it means to recover from such an invasive procedure amidst the chaos of life outside those sterile walls.
A Framework for Moving Forward
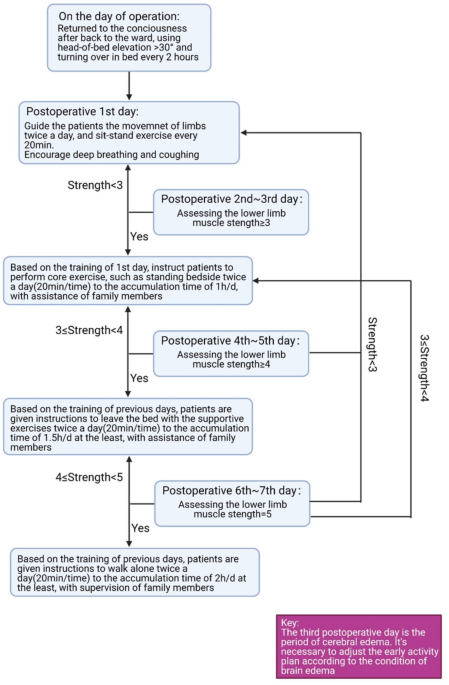
You know what’s fascinating? The early mobilization protocol I followed felt almost like choreography in a rhythm where every move mattered. On the day after surgery, with my head elevated at 30 degrees—my heart raced with anticipation as nurses assisted me in turning over every two hours. There’s something surreal about realizing you’ve become part of someone else’s routine—a mere cog in their grand machine—but also pivotal to your own healing.
I’ll never forget sitting up in bed for twenty minutes twice daily—it seemed trivial at first glance. But each moment spent exercising my limbs felt monumental; it was reclaiming agency over my body when everything else felt shaky at best.
“Victory belongs to the most persevering!” This mantra echoed around me—where did they find all these uplifting sayings? In moments when doubt crept in, those words became tiny beacons guiding me through foggy days.
Navigating Pain and Progress
Pain management isn’t exactly glamorous, is it? Multimodal analgesia sounds sophisticated—a hodgepodge of strategies designed to tackle discomfort from multiple angles—but let’s be real: sometimes all you want is relief without feeling like you’re floating through life on cloud nine or trapped beneath its weight. Nurses would ask if my pain score hit two or above—I remember hesitating before answering because admitting pain often feels like vulnerability laid bare.
This brings us to psychological support—a quiet hero amidst clinical jargon that sometimes feels devoid of empathy. When someone sat down next to me asking about my worries rather than how much pain I was in—that made all the difference! Anxiety can sneak up on you post-surgery; suddenly being discharged can feel more daunting than facing surgery itself.
An Infrastructure for Independence
You’d think recovering from brain surgery would mean lying quietly in bed while someone fusses over you—but oh no! The hospital had transformed itself into an arena where independence thrived! Handrails lined corridors inviting us to pull ourselves up instead of sinking back down into helplessness.
A walking aid became less about dependence and more about empowerment—each step forward ushered feelings from despair towards potential renewal. Yet still…didn’t anyone else feel overwhelmed by their own pace? Why does recovery have such lofty expectations attached?
The Never-Ending Chase for Outcomes
I couldn’t help but ponder outcome variables during those monotonous stretches between physical therapy sessions—their significance weighed differently depending upon whom you asked: clinicians aiming high while we patients trudged along wanting simple validations around activities of daily living (ADLs) instead.
For instance: How do we truly measure success? Is it reduced length-of-stay or fewer complications post-discharge? Or is it simply getting back home again without feeling lost?
A Personal Reflection
No neat endings here—just echoes lingering long after leaving that ward behind me—what remains are memories stitched together with resilience despite uncertainty looming ahead. As time unfolds layers upon layers beyond surgical scars lies revelation: recovery doesn’t happen overnight nor within confines defined by clinical outcomes alone!
[1] ERAS Society Neurosurgical Guidelines
[2] Katz’s Activities of Daily Living Index
Written for Aging Decoded – The Future of Health News, One Story at a Time.